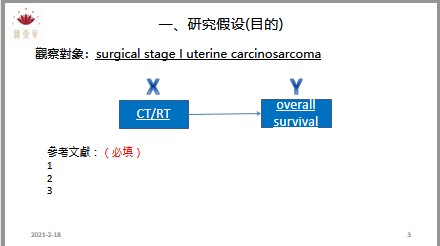
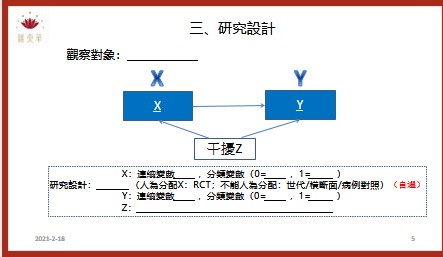
Researchers measured the effect on one year mortality of secondary drug prevention for patients with stroke in routine primary care. They used a cohort study design, which incorporated patient data from the health improvement network primary care database. Participants were 12 830 patients aged 50 years or more from 113 general practices. They had all had a stroke between 1995 and 2005 and survived the first 30 days after the stroke. Secondary drug prevention was defined as being prescribed either antihypertensives plus lipid lowering drugs plus ntithrombotics or antihypertensives plus lipid lowering drugs.1
Cox proportional hazards regression was used to investigate one year mortality, defined as death from any cause from 31 days after the stroke and within the first year. Univariable and multivariable analyses between one year mortality and secondary drug prevention, sex, socioeconomic deprivation, and age group were performed (table⇓). Socioeconomic deprivation was measured by the Townsend score, which assesses socioeconomic deprivation in families and includes measurement of employment status, overcrowding, car ownership, and owner occupation status.
On average, mortality within the first year was 5.7% for patients receiving secondary drug prevention compared with 11.1% for patients not receiving treatment. Secondary drug prevention
was associated with a 50% reduction in mortality risk (adjusted hazard ratio 0.50, 95% confidence interval 0.42 to 0.59).
Which of the following statements, if any, are true?
a) The outcome variable for the Cox proportional hazards regression was continuous
b) The hazard ratio predicts the relative proportions of patients who will have died in the categories of each variable at the end of follow-up
c) It was assumed that for each category of the explanatory variables the hazard of death was constant during follow-up
d) It can be concluded that secondary drug prevention was independently associated with one year mortality
 匯東華統計顧問有限公司
匯東華統計顧問有限公司 
![]()
![]()

![]()
![]()